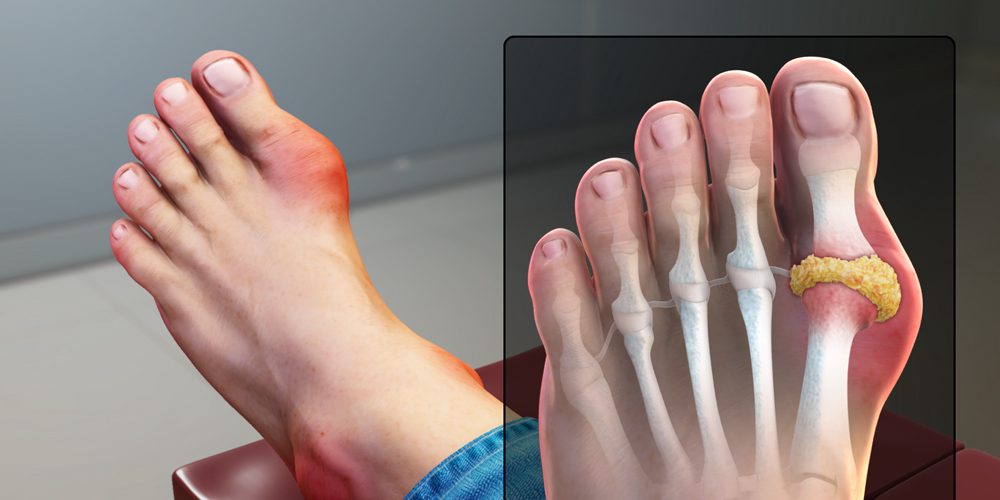
Gout is a severe and complex type of arthritis that affects everyone. It’s got such an unpleasant name for a reason: it’s characterized by extremely painful, swollen, red and warm feelings in one or more joints, typically the big toe.
Gout, like other acute rheumatic diseases, can strike suddenly and dramatically. Frequently, you will wake up in the middle of the night with a burning sensation in your big toe. The afflicted joint is hot, swollen, and extremely sensitive that even the weight of a bedsheet on it may be painful.
Gout symptoms may vary in severity, but there are several techniques for coping with them and preventing recurrences.
This article is a part of our foot pain series. If you want to read more about other foot disorders, please visit our main article here.
Symptoms of Gout
The most typical indications and symptoms of gout generally appear suddenly and usually at night. They include:
- Intense pain in the joint. Gout generally affects the big toe, although it may affect any joint. The ankles, knees, elbows, wrists and fingertips are among the most frequently affected joints. The pain is likely to be most severe within the first four to 12 hours after it begins.
- Lasting discomfort. Joint discomfort may last for a few days to a few weeks after the most severe pain has subsided. Later episodes are more prone to linger and affect additional joints.
- Reduced range of motion. The affected joint may abruptly become stiff or swollen, limiting your range of motion.
- Extreme heat in the joint. Early on, your skin over the most afflicted area might seem hot to the touch. This heat usually diminishes after a few hours and is replaced by intense pain, which you’ll notice when touching the affected part of your body or when a doctor presses on it.
- Swollen, inflamed, and reddened skin. The skin surrounding your joint may appear puffy and swollen. It may become flushed, red, or dark purple. If you have dark skin, the affected area might instead appear greyish blue.
What causes gout?
Gout is an illness in which urate crystals build up in your joint, triggering the pain and swelling associated with a gout attack. When you have high levels of uric acid in your circulation, urate crystals may develop. When your body breaks down purines it produces uric acid, chemical compounds found naturally within your body.
Purines are present in a variety of foods, including red meat and organ meats such as liver. Anchovies, sardines, mussels, scallops, trout and tuna are all high in purine. Alcoholic beverages, particularly beer, and drinks sweetened with fruit sugar (fructose) raise uric acid levels.
Normally, uric acid dissolves in the blood and carried by the kidneys to your urine. However, if either your body or your kidneys produce too much uric acid, or if they excrete too little, uric acid can build up in a joint or surrounding tissue, causing discomfort, swelling, inflammation and pain.
What Increases Your Risk For Gout?
You have already discovered the relation between uric acid and gout. This means that your risk of getting gout at some point in your life increases with the levels of uric acid your body produces. The main factors leading to higher uric acid levels include:
- Food and Diet. Gout is more common in individuals who eat a diet high in red meat and shellfish, as well as those who drink sweetened beverages containing fruit sugar (fructose). The risk of gout is higher among people who consume alcohol.
- Age and gender. Gout occurs more frequently in males, owing to the fact that women have generally lower uric acid levels. However, after menopause, women’s uric acid levels begin to approach those of males. Gout is more likely to strike earlier in men (usually between the ages of 30 and 50) than it does in women, who usually show symptoms after menopause.
- Your Weight. Being overweight causes a lot of health problems. I am sure you already know that. No wonder that this affects gout as well. The more weight you carry, the harder it gets for your kidneys to eliminate uric acid and the more uric acid is being produced.
- History of gout in your family. It’s not clear if gout can be inherited, but if other family members have had gout, you’re more likely to develop this disease too.
- Medical conditions. Gout is more likely in individuals who have diseases or conditions that increase their risk. Untreated high blood pressure and chronic illnesses including diabetes, obesity, metabolic syndrome, and heart and kidney diseases are all risk factors.
- Medications. Low-dose aspirin and certain antihypertensive medications, such as thiazide diuretics, angiotensin-converting enzyme (ACE) inhibitors, and beta blockers, all can raise uric acid levels. Also, the use of anti-rejection medicines for those who have had an organ transplant can cause this disease.
- Trauma or recent surgery. Recent surgery or trauma can occasionally trigger Gout attacks. In certain individuals, a vaccination might cause a gout flare.
Diagnosis
A doctor or a group of specialists that specialize in treating gout patients should establish the diagnosis and therapy. This is critical since the signs and symptoms of gout are nonspecific, mimicking those of other inflammatory diseases. Rheumatologists are doctors who specialize in gout and other types of arthritis. The American College of Rheumatology’s database of rheumatologists can help you locate a specialist near you. Common tests to diagnose gout include:
- Blood test. A blood test is one of the most frequent tests to evaluate your uric acid levels. However, blood test findings can be deceptive. Some people have excessively high uric acid levels but never develop gout. Some individuals have gout symptoms but no unusual amounts of uric acid in their blood.
- X-Ray Imaging. Mainly used to rule out other joint inflammation causes, X-Rays can be very helpful.
- Test of joint fluid. A needle extracts fluid from the affected joint if your doctor feels it is needed. When the fluid is examined under a microscope, urate crystals may be visible.
- Ultrasound. Sound waves can be a good way to detect urate crystals in your joints.
- Dual-energy computerized tomography (DECT). This test is a combination of X-Ray images from different angles to visualize urate crystals in your joints.
Treatment
Gout can be successfully treated and managed with medication and self-care procedures. A medical treatment plan might be recommended by your doctor.
Gout medications are available in two forms, each with its own focus. The first type targets the inflammation and discomfort that accompany gout attacks. The second type goal is to prevent gouts by lowering uric acid levels in your blood.
The frequency and severity of your symptoms, as well as any other health issues you may have determine the type of medication that’s appropriate for you.
Medications to treat gout flares and future attacks
The most common medications used to treat gout attacks and prevent future occurrences include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Over-the-counter alternatives include ibuprofen (Advil, Motrin IB, and others) and naproxen sodium (Aleve), as well as stronger prescription NSAIDs like indomethacin (Indocin, Tivorbex) or celecoxib (Celebrex).
- Colchicine. Your doctor may prescribe colchicine (Colcrys, Gloperba, Mitigare), an anti-inflammatory medication that helps to relieve gout symptoms. However, the drug’s efficiency may be offset by side effects such as nausea, vomiting, and diarrhea.
- Corticosteroids. Prednisone, for example, is a corticosteroid that can help with gout inflammation and pain. Corticosteroids can be taken as pills or injected into the joint. Mood swings, increased blood sugar levels and high blood pressure are potential side effects of corticosteroids.
Medications to prevent gout getting worse
If you have frequent gout attacks or if your gout episodes are less severe but excruciating, your doctor may prescribe medicine to help you avoid gout-related problems. If you have gout on X-rays or tophi, chronic kidney disease or kidney stones, your doctor may prescribe medications to lower your body’s level of uric acid.
- Uric acid production blockers. Allopurinol and febuxostat (Uloric) are medications that limit the amount of uric acid your body makes. Allopurinol has several negative effects, including a fever, rash, hepatitis and kidney issues. Febuxostat may cause a rash, nausea, and decreased liver function. Heart-related death is also increased by febuxostat.
- Uric acid removers. Strengthening your kidneys’ ability to remove uric acid is helped by medicines such as probenecid (Probalan). A rash, stomach discomfort, and kidney stones are some of the side effects.
In addition to medical therapy, you can control your gout by using self-management techniques. Self-management is a term used to describe your everyday efforts to manage your condition and stay healthy, such as making nutritious lifestyle decisions. The self-management tips outlined below have been shown to reduce pain and disability, allowing you to enjoy the activities that matter most to you.
Lifestyle changes and home remedies
Gout has a variety of daily living impacts, including job and leisure activities. Fortunately, numerous low-cost self-management options have been shown to enhance gout patients’ quality of life. Here are the top tips that have the best success rates:
- Eat fresh and healthy. Avoid foods that may cause a gout flare, such as high-purine meals (such as a red-meat diet), and drinking alcohol in moderation (particularly beer and strong spirits).
- Choose healthy beverages. Alcoholic beverages and drinks sweetened with fruit sugar (fructose) should be avoided. Instead, drink a lot of nonalcoholic fluids, especially water.
- Consider losing some weight and exercise regularly. Keeping a healthy weight reduces your chance of getting gout. Choose low-impact activities like walking, cycling, and swimming to help you avoid injuring your joints.
- Protect your joints. Arthritis sufferers should avoid activities that place a lot of strain on their joints, such as running or horseback riding. Running and horseback riding can cause or exacerbate joint problems. Walking, bicycling, and swimming are all easy on the joints and have a low risk of harm.
- Learn self-management skills. Join a self-management education program to learn how arthritis affects your life and increase your confidence in controlling your symptoms and living well.
- Get active. 150 minutes of at least moderate physical activity is recommended for adults on a weekly basis. Every minute spent exercising adds up, and any form of movement beats none. Walking, swimming and cycling are all good low-impact hobbies. Physical exercise can help to lower the chances of developing other chronic diseases such as heart disease, stroke, and diabetes. Learn more about arthritis physical activity.
- Join physical activity programs. For those who worry that physical activity might aggravate their arthritis or don’t know how to exercise securely, participation in organized activities may help them reduce discomfort and disability linked to arthritis while also improving mood and mobility. Classes are offered in public spaces such as parks and community centers. These classes might help persons with arthritis feel more comfortable.
- Engage with your doctor. By visiting your regular medical appointments and following your prescribed treatment plan, you can take an active part in managing your arthritis. This is especially crucial if you have additional persistent illnesses, such as diabetes or heart disease.
Takeaways
The main takeaway is that, while there is no cure for gout, it can be managed effectively with medication and self-management strategies. The medical tips above are the ones that have the best success rate for helping people to manage their condition. There are also many lifestyle changes and home remedies that one can use to help themselves if they don’t want to use medication.
Are you looking for products to help protect your joints? Browse our shop, where you can find knee braces, socks, compression sleeves and more! And as always, we’d like to hear your thoughts and experiences, so please don’t hesitate to comment below.