Patrick Haglund first described the condition in 1927. It is also known as retrocalcaneal exostosis, Mulholland deformity, and ‘pump bump.’ It’s a very common clinical issue, but it’s still poorly understood.
What is Haglund’s Deformity?
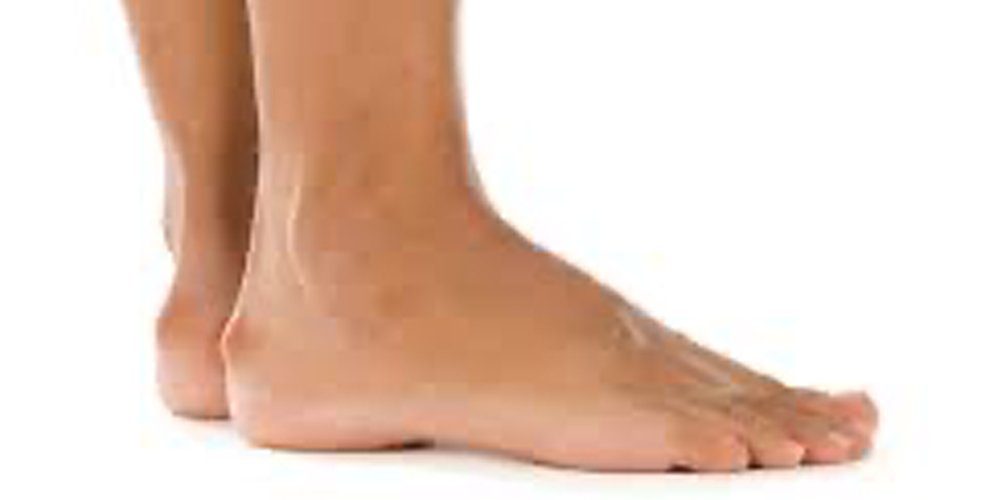
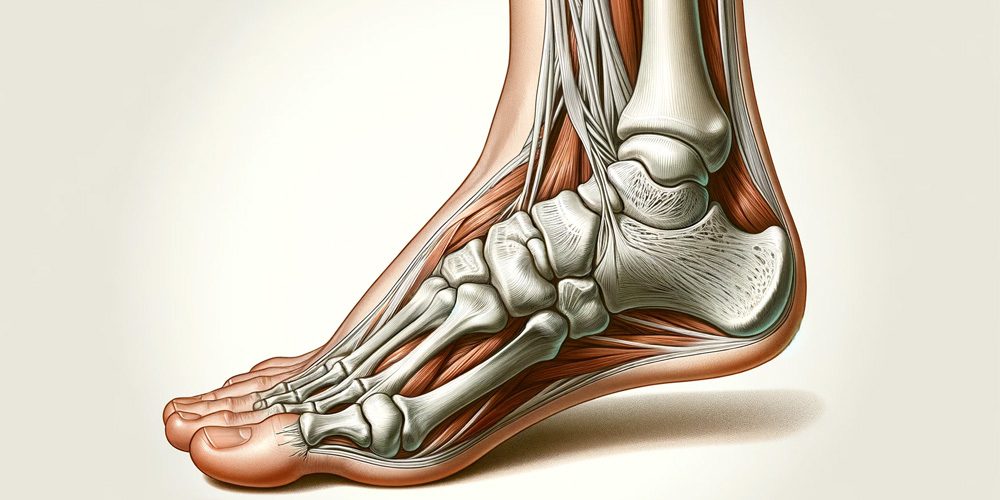
Haglund’s deformity is a bone and soft-tissue abnormality of the foot. This condition is caused by an expansion in the bony portion of the heel (where the Achilles tendon is inserted). When rigid shoes rub against the large, bony lump near the rear of the heel, it can irritate the soft tissue nearby. This can lead to painful bursitis, an inflammation of the bursa (a fluid-filled sac between the tendon and bone). Anyone can get Haglund’s deformity. It happens most often in people who wear hard, closed-heel shoes.
Symptoms
One or both feet can be afflicted with Haglund’s deformity. The following are some of the signs:
- A noticeable bony bump at the back of your heel
- Severe pain in the area where your Achilles tendon attaches to the heel
- Swelling in the bursa at the back of your heel
- Redness in the area of the inflamed tissue
Causes
When you apply pressure to the backs of your heels frequently, Haglund’s deformity occurs. It’s most likely caused by wearing shoes that are too tight or rigid in the heel. Haglund’s deformity, which is often known as “pump bump,” develops in females who wear pump-style high heels.
If you have a high foot arch, a tight Achilles tendon, or tend to walk on the outside of your heel, you may be more prone to Haglund’s deformity.
Diagnosis
Because the signs of Haglund’s deformity are comparable to those of other foot problems, including Achilles tendonitis, it might be difficult to identify.
Your doctor may be able to determine the problem based on the appearance of your heel. If your physician suspects you have Haglund’s deformity, they may recommend an X-ray of your heel bone. This will assist your doctor in determining whether you have the disease’s characteristic heel bone.
An X-ray may also aid your doctor in creating orthotics to help you manage your heel discomfort. Orthotics are personalized shoe inserts used to maintain the health of your feet.
Non-Surgical Treatment
Haglund’s deformity is usually treated with a combination of therapies that focus on reducing discomfort and relieving pressure off your heel bone. Non-surgical treatments include:
- Wearing shoes with an open-heel design, such as clogs or sandals
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs). These include Ibuprofen (Advil, Motrin IB) or Aspirin (Bufferin)
- Applying ice packs to the bump for 20-40 minutes per day. This is done to reduce swelling
- Ultrasound treatments as part of a physical therapy
- Soft tissue massages
- Wearing orthotics is a great way to cushion the heel
- Heel pads reduce the pressure from shoes
- Compression socks can be helpful to improve blood circulation and reduce swelling
- Wearing a cast or immobilization boot
- A night splint can help reduce pain overnight
Surgery
Haglund’s deformity can also be treated by surgery, whether less invasive techniques fail to work. Your doctor will remove the extra bone from your heel during surgery. The bone may also be smoothed and filed down to decrease pressure on the bursa and soft tissue.
Depending on the nature and extent of your injury, you may be administered a general anesthetic to put you to sleep throughout the operation. If your Achilles tendon is broken and needs to be restored, this is typically done.
Following surgery, it might take up to eight weeks for you to heal completely. Your doctor will most likely prescribe a boot or cast to protect your foot. You may possibly need to use crutches for a few days or weeks following the operation.
The incision will need to be kept bandaged for at least seven days. Your stitches will be removed after two weeks if your surgeon is happy with the healing progress. Your doctor might want to take an X-ray of your foot on later visits to make sure it’s healing properly.
Prevention
You may reduce your chance of developing Haglund’s deformity by properly caring for your feet. A recurrence may be prevented by:
- Wearing appropriate shoes
- Avoiding shoes with a rigid heel back
- Using arch supports or heel pads in shoes
- Wearing proper orthotic devices
- Avoiding hard surfaces and running uphill
- Performing stretches and exercises that relieve tension from the Achilles tendon
- Regularly participating in physical therapies
- Wearing padded socks or socks with non-slip soles
Takeaways
Your discomfort should go away with adequate therapy. While some sufferers may see their symptoms return, adopting the measures outlined above can help you avoid having Haglund’s deformity again.
If you have had Haglund’s Deformity and have successfully treated this condition, please comment your story below and let us know what methods and lifestyle changes worked best for you.
If you’re looking for insoles, orthotics, splints or compression socks to treat your foot pain, please have a look at our products. They’ve already helped thousands of customers from all around the world.