Picture this: You’re up with the sun, lacing your running shoes, ready to greet the day with a refreshing morning jog. But the moment your foot hits the pavement, a sharp, stabbing pain shoots through your heel. You wince, hobbling back inside. The culprit? Plantar Fasciitis.
Welcome, dear reader, to our deep dive into this all-too-common foot ailment. You might be wondering, “Plantar what now?” Don’t worry, we’re here to shed light on this mysterious condition that’s been the bane of athletes, office workers, and morning joggers alike.
Plantar Fasciitis, a name that sounds like it belongs to an exotic plant species, is actually a common foot condition that affects 1 in 10 people at some point in their lives. It’s the invisible gremlin that turns a simple step into a grimace-inducing ordeal.
But fear not, for we’re about to embark on a journey to understand this condition, its causes, and most importantly, how to send it packing. We’ll explore the latest research, debunk common myths, and arm you with knowledge so you can stride confidently forward.
So, whether you’re a seasoned marathoner, a weekend warrior, or someone who just enjoys a leisurely stroll, this blog post is for you. Because let’s face it, we all deserve to walk, run, and dance without pain.
Stay with us as we unravel the mystery of Plantar Fasciitis, the silent disruptor of your daily life. By the end of this post, you’ll be well-equipped to tackle this condition head-on, and reclaim your active lifestyle.
The Painful Truth: Understanding Plantar Fasciitis
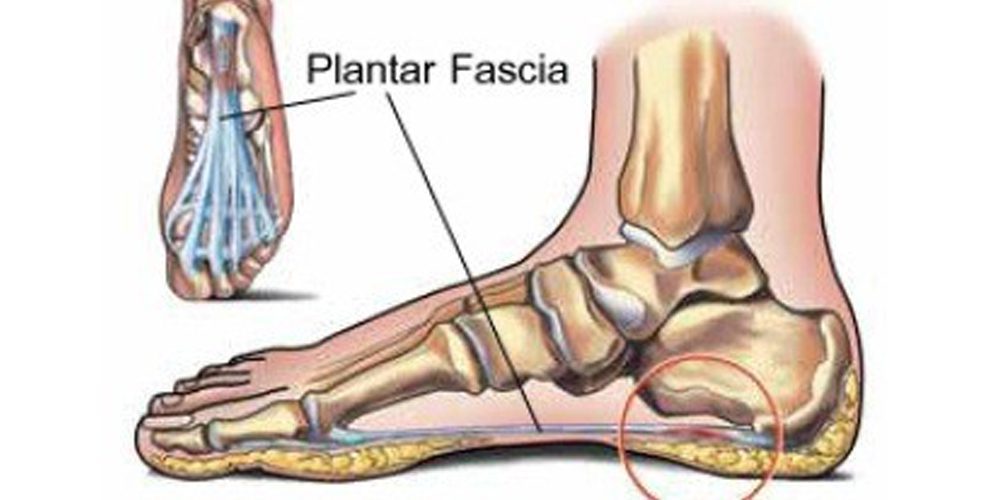
Plantar fasciitis is a common foot condition that causes pain and discomfort in the heel and sole of the foot. The plantar fascia is a thick band of tissue that connects your heel bone to your toes, and it supports the arch of your foot.
When this tissue becomes inflamed, it leads to plantar fasciitis. This condition affects millions of people around the world, and if left untreated, it can lead to chronic pain.
How Plantar Fasciitis Affects People
Plantar fasciitis can have a significant impact on someone’s daily life. It can cause severe pain in the heel or arch of the foot, making it difficult to walk or stand for long periods. The pain is usually worse in the morning or after periods of rest when you first step out of bed or stand up after sitting for a while.
The discomfort caused by plantar fasciitis can also affect an individual’s ability to exercise or play sports that involve running or jumping. This lack of physical activity may lead to weight gain and other health problems.
The Importance of Understanding Plantar Fasciitis
It is essential for people to understand this condition because early intervention can prevent long-term consequences such as chronic pain and disability. Knowing what causes plantar fasciitis may help individuals take steps towards preventing its onset. In addition, understanding how plantar fasciitis affects daily life can help individuals make necessary adjustments such as wearing proper footwear and avoiding activities that put excessive stress on their feet.
Awareness about this condition is also crucial because many people mistakenly believe that plantar fasciitis will resolve on its own without any treatment. This is not true; without proper care, the condition can worsen over time and lead to additional complications.
Understanding plantar fasciitis can provide relief and comfort to those who are affected by it. Knowledge about the condition can empower individuals to take charge of their health and seek appropriate medical attention.
Plantar fasciitis is a painful foot condition that affects millions of people worldwide. It can have a significant impact on an individual’s daily life and well-being. Understanding the causes, symptoms, and treatment options for this condition is crucial for early intervention and long-term prevention of chronic pain and disability.
What is Plantar Fasciitis?
Plantar fasciitis is a condition that affects the plantar fascia, a thick band of tissue that runs along the bottom of your foot. This tissue connects your heel bone to your toes and supports the arch of your foot.
When this tissue becomes inflamed or irritated, it can cause pain in the heel or arch of the foot. The pain is typically described as a sharp stabbing sensation that is worst in the morning and after periods of rest.
Plantar fasciitis is one of the most common causes of heel pain, affecting approximately 10% of people at some point in their lives. It can be a chronic condition if left untreated, but with proper treatment, most people experience significant relief from their symptoms.
Causes and Risk Factors
The exact cause of plantar fasciitis is not fully understood, but there are several factors that can increase your risk for developing this condition. One major risk factor is age; plantar fasciitis tends to occur more frequently in people over 40 years old.
Other risk factors include: – Obesity: Carrying excess weight puts extra stress on your feet and can increase your risk for developing plantar fasciitis.
– Overuse: Activities that involve repetitive impact on your feet, such as running or jumping, can put stress on your plantar fascia and lead to inflammation. – Foot structure: People with high arches or flat feet are at an increased risk for developing plantar fasciitis.
– Tight calf muscles: Tightness in the muscles at the back of your leg can put extra strain on your plantar fascia. – Certain occupations: Jobs that require standing for long periods or walking on hard surfaces may increase your risk for developing plantar fasciitis.
In some cases, plantar fasciitis can also be a result of a more serious underlying condition such as rheumatoid arthritis or nerve entrapment. It’s important to speak with your doctor if you are experiencing persistent foot pain to rule out any other underlying conditions.
Symptoms of Plantar Fasciitis
Now that we’ve set the stage, let’s delve into the heart of the matter. Here are the most common symptoms of plantar fasciitis.
The Pain
Plantar fasciitis is typically characterized by a sharp, stabbing pain in the heel or arch area of the foot. This pain usually develops gradually, and may be particularly acute after periods of inactivity, such as when first getting out of bed in the morning or after prolonged sitting.
As the condition progresses, this pain may become more chronic and persistent. This is because over time, inflammation can develop within the plantar fascia tissue itself.
Tightness or Stiffness
Another common symptom of plantar fasciitis is a feeling of tightness or stiffness in the bottom of the foot. This is often most noticeable upon waking up in the morning or after long periods of sitting. The tightness may feel like a dull ache that radiates through the entire foot.
Swelling
Swelling can also occur with plantar fasciitis, especially during acute flare-ups. Swelling may be visible around the heel area or along the arch of your foot. If you notice any swelling, it’s essential to take steps to reduce inflammation right away to help avoid worsening symptoms.
Difficulty Walking Normally
Because plantar fasciitis affects one’s ability to put weight on their affected foot without experiencing severe pain, many people find themselves walking with a limp or favoring one side over another when walking. Over time and without proper treatment, this can lead to altered gait patterns and even additional injuries due to compensatory movements made by other parts of your body.
Numbness or Tingling Sensations
In some cases, individuals with plantar fasciitis may experience numbness or tingling sensations along their affected foot’s bottom. This sensation can indicate that nerves within your feet are being compressed or irritated by the inflamed tissues in your feet. If you experience these symptoms, it’s crucial to speak with your doctor immediately to identify any underlying nerve damage and begin treatment as soon as possible.
Recognizing the Symptoms
The key to addressing plantar fasciitis is understanding its symptoms and getting a proper diagnosis early on. If you’re experiencing any of the above-listed symptoms, it’s critical to take steps right away to reduce inflammation and provide relief for your feet. Speak with your doctor or a foot specialist today for more information about the best ways to manage plantar fasciitis and protect your long-term foot health.
Diagnosis of Plantar Fasciitis
Now that we got the symptoms down, it’s important to confirm your suspicions.
How doctors diagnose plantar fasciitis
Plantar fasciitis can be diagnosed by a medical professional, such as a podiatrist or orthopedist, through a combination of physical examination and medical history. The doctor will begin by asking about any symptoms the patient is experiencing, taking note of when they began and their severity. They will then perform a physical examination, which typically includes assessing the foot’s range of motion and checking for any areas of pain or tenderness.
During the exam, the doctor may also assess the patient’s gait to look for any abnormalities that could be contributing to their condition. They may ask the patient to walk barefoot or in different types of shoes to evaluate how their foot moves.
Medical tests used for diagnosis
In addition to a physical exam, there are several medical tests that can be used to diagnose plantar fasciitis. These include X-rays and ultrasounds.
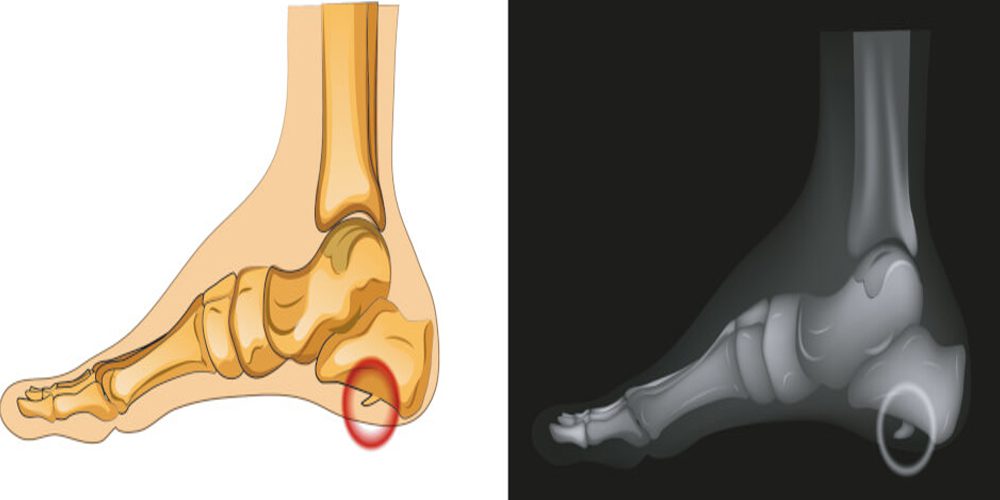
X-rays can help rule out other conditions that may be causing foot pain, such as stress fractures or arthritis. While they cannot directly show plantar fasciitis itself because soft tissue does not show up on X-ray images, they can help identify bone spurs that are sometimes associated with this condition.
Ultrasound imaging is another diagnostic tool used to detect plantar fasciitis. It uses high-frequency sound waves to create images of internal structures in the body.
An ultrasound can provide a detailed view of the soft tissues in and around the heel area, allowing doctors to see if there is inflammation or thickening in the plantar fascia. MRI (Magnetic Resonance Imaging) scans are also used if there is doubt about diagnosis after other tests have been completed or indication towards surgery needs further confirmation about type of surgery required.
After obtaining diagnostic imaging information and evaluating physical exam results, the doctor will determine whether the patient has plantar fasciitis and what treatment options are best suited for their individual condition. It is important for patients to seek medical attention if they experience foot pain or other symptoms related to plantar fasciitis, as early detection and intervention can prevent the condition from worsening.
Treatment Options for Plantar Fasciitis
Ok, you got your answer. Plantar fasciitis is identified and confirmed. Now what?
Non-surgical treatments such as stretching exercises, physical therapy, and orthotics
Plantar fasciitis can be treated non-surgically. Stretching exercises are one of the most effective treatments for plantar fasciitis. These exercises help to strengthen the muscles of the foot and lower leg, improve flexibility, and reduce pain.
Physical therapy is often recommended for severe cases of plantar fasciitis. A physical therapist will work with the patient to develop a customized exercise program designed to address their specific needs.
Orthotics are another non-surgical treatment option for plantar fasciitis. Orthotics are shoe inserts that are designed to provide support and cushioning for the feet.
They can help to redistribute pressure on the foot and reduce pain associated with plantar fasciitis. Rest is also an important part of treating plantar fasciitis.
It is important to avoid activities that exacerbate symptoms of pain and discomfort in the feet. Wearing shoes with good arch support, avoiding high heels or flip-flops can also help alleviate symptoms.
Surgical options for severe cases
In severe cases where non-surgical treatments have not been effective in relieving symptoms or improving quality of life, surgical procedures may be considered as treatment options. One surgical option is called a plantar fasciotomy which involves cutting part of the plantar fascia ligament in order to relieve tension on it.
Another procedure is called gastrocnemius recession where incisions made at calf muscles so they lengthen which reduces stress on feet’s soles. Surgery should be considered as a last resort after all other treatment options have been exhausted due to potential risks associated with surgery including complications from anesthesia and postoperative infections.
It’s important for individuals who may be considering surgery as a treatment option for their plantar fasciitis to consult with a qualified orthopedic specialist. They can discuss surgical risks and help determine whether or not surgery is the best course of action for treating their condition.
Prevention Strategies for Plantar Fasciitis
Understanding the symptoms and diagnosis of Plantar Fasciitis is half the battle. The other half? Preventing it from gatecrashing your life in the first place.
Lifestyle changes that can help prevent plantar fasciitis
Plantar fasciitis can be a painful and debilitating condition that can significantly affect a person’s quality of life. While there are several treatment options available to manage the condition, prevention strategies are equally important.
Making lifestyle changes is one way to reduce the risk of developing plantar fasciitis. One of the most effective ways to prevent plantar fasciitis is to maintain a healthy weight.
Carrying excess weight puts extra strain on the feet, which can cause inflammation in the plantar fascia. Losing weight through diet and exercise can help reduce this strain and lower the risk of developing plantar fasciitis.
Another lifestyle change that can help prevent plantar fasciitis is maintaining good foot health. This includes keeping feet clean and dry, trimming toenails regularly, and wearing proper footwear.
Taking care of your feet reduces the risk of developing infections or other conditions that may lead to foot pain or discomfort. Stretching exercises are also essential in preventing plantar fasciitis.
Stretching helps strengthen muscles, improve flexibility, and increase range of motion in the feet. It is recommended to perform calf stretches twice a day, holding each stretch for at least 30 seconds.
Proper footwear choices
Wearing proper footwear is crucial in preventing plantar fasciitis. Shoes that provide adequate support for arches and heels help reduce stress on the feet and minimize inflammation in the plantar fascia.
Shoes with good shock absorption also protect against impact forces during physical activity. It is important to choose shoes that fit well and provide enough room for toes to move freely inside them.
Tight-fitting shoes or those with pointed toes should be avoided as they may cause pressure on certain areas of the foot leading to pain or discomfort. Orthotics or shoe inserts can also be helpful in preventing plantar fasciitis.
They are designed to provide extra support and cushioning to the feet, minimizing stress on the plantar fascia. Custom-made orthotics can be prescribed by a podiatrist for individuals with specific needs.
There are several lifestyle changes that can help prevent plantar fasciitis. Maintaining a healthy weight, taking care of foot health, and performing stretching exercises regularly are essential in reducing the risk of developing the condition.
Choosing proper footwear with adequate support and cushioning is equally important in protecting the feet from stress and inflammation. By adopting these prevention strategies, individuals can minimize their chances of developing plantar fasciitis and enjoy an active lifestyle free from foot pain or discomfort.
The Connection Between Obesity and Plantar Fasciitis
You might be wondering, “What does my weight have to do with my foot pain?” Unfortunately, the connection might be stronger than you think.
Obesity increases the risk of developing plantar fasciitis
Plantar fasciitis is a painful condition that affects the foot’s plantar fascia, which is a thick band of tissue that connects the heel bone to the toes. Obesity has been identified as a significant risk factor for developing plantar fasciitis.
The increased weight puts extra pressure on the foot, making it more susceptible to injury and damage to the plantar fascia. Additionally, obese individuals are often less physically active, which can also contribute to an increased risk of developing plantar fasciitis.
A study published in The Journal of Bone and Joint Surgery found that overweight individuals were more likely to experience heel pain and develop plantar fasciitis than those who were not overweight. Another study published in Foot & Ankle International found that those with a body mass index (BMI) over 30 had an almost three times greater risk of developing plantar fasciitis compared to those with a BMI between 18.5 and 24.9.
Tips for weight management to reduce the risk
Maintaining a healthy weight is crucial for preventing or managing numerous health conditions, including plantar fasciitis. Losing weight can help reduce pressure on your feet and lower your risk of developing this painful condition.
One effective strategy is adopting a healthy diet that emphasizes whole foods such as fruits, vegetables, lean proteins, and whole grains while avoiding processed foods high in sugar or unhealthy fats. Regular exercise can also help manage weight by burning calories, building muscle mass, and improving overall fitness levels.
Incorporating strength training exercises into your routine can also be helpful for reducing your risk of developing plantar fasciitis. Strengthening muscles around your feet and ankles can help improve stability while reducing stress on the plantar fascia.
Another useful weight management tip is to consult with a healthcare professional or registered dietitian for personalized advice on nutrition and exercise plans tailored to your individual needs and goals. Small modifications to lifestyle habits such as taking the stairs instead of the elevator, parking farther away from destinations, and reducing screen time can also contribute to improved overall health and weight management.
Plantar fasciitis is a painful condition that can significantly impact one’s quality of life. Obesity is a significant risk factor for developing plantar fasciitis, but there are numerous strategies for managing weight and reducing the risk of this condition.
By adopting healthy lifestyle habits that include regular exercise, strength training, and balanced nutrition choices, individuals can maintain a healthy weight while improving overall health outcomes. Consultation with healthcare professionals can also be helpful in creating personalized plans that take into account individual needs and goals.
The Role of Genetics in Plantar Fasciitis
As obesity can be a factor that promotes plantar fasciitis, your genes could also play a role.
Genetics and the Development of Plantar Fasciitis
Plantar fasciitis is a common condition that affects many people, and while there are several risk factors that can contribute to its development, genetics may also play a role. Research has shown that certain genes may increase an individual’s susceptibility to developing the condition, even in the absence of other known risk factors. However, much more research is needed to fully understand the relationship between genetics and plantar fasciitis.
Family History and Plantar Fasciitis
One way in which genetics may be linked to plantar fasciitis is through family history. Studies have found that individuals who have a family member with plantar fasciitis are more likely to develop the condition themselves. This suggests that there may be genetic factors at play, although it’s important to note that other factors such as lifestyle choices and environmental exposures can also contribute.
Genetic Markers and Plantar Fasciitis
Another area of research on genetics and plantar fasciitis has focused on identifying specific genetic markers associated with the condition. One study conducted by researchers at Harvard Medical School identified several genes related to inflammation and tissue repair that were more prevalent in individuals with plantar fasciitis compared to those without. This suggests that these genes may be involved in the development or progression of the condition.
Implications for Treatment and Prevention
While much more research is needed in this area, understanding how genetics may contribute to plantar fasciitis could have important implications for treatment and prevention strategies. For example, if certain genetic markers are found to increase an individual’s risk for developing the condition, screening tests could be developed to identify those at higher risk early on. Additionally, treatments or preventative measures could be tailored to an individual’s genetic profile.
Future Directions for Research
Overall, there is still much to learn about the role of genetics in plantar fasciitis. More research is needed to fully understand how genetic factors interact with environmental and lifestyle risk factors, and whether or not screening tests or personalized treatment approaches could be beneficial. However, by continuing to explore this area of study, we may be able to better understand and effectively treat this common condition.
Common Misconceptions about Plantar Fasciitis
When you speak about your conditions, you might be confronted with all kinds of different opinions, advice or stories. I want to encourage you to not care about those opinions too much. Here are the most common misconceptions and myths about plantar fasciitis.
The Pain is All in Your Head
One common misconception about plantar fasciitis is that the pain experienced is all in the head. People may assume that if there’s no visible injury or swelling, then there must not be any actual pain.
However, plantar fasciitis is a real condition with real symptoms. The pain can be debilitating and can make daily activities difficult to perform.
Resting and Doing Nothing Will Cure Plantar Fasciitis
Another common myth about plantar fasciitis is that it will go away on its own if you simply rest and do nothing. In reality, this condition requires active treatment to fully heal. Resting too much can actually make the condition worse by causing the muscles and tendons in your feet to become weaker.
Only Athletes Get Plantar Fasciitis
While athletes are more prone to developing plantar fasciitis due to the strain on their feet from sports activities, anyone can develop this condition. It’s important not to assume that only those who engage in high-intensity physical activity are at risk.
Plantar Fasciitis Only Affects Older Individuals
It’s also a common misconception that only older individuals get plantar fasciitis. In reality, this condition can affect people of all ages, including children and young adults.
Conclusion
Plantar fasciitis is a painful and often misunderstood condition that affects many people worldwide. It’s important for individuals to understand exactly what this condition entails and how best to treat it.
With proper knowledge, preventative measures like wearing supportive footwear or maintaining a healthy weight may help ward off an attack of plantar fascia strains or tears as well as help avoid misconceptions regarding its nature. While plantar fasciitis can be a challenge to manage, with the right approach and mindset, individuals can take steps towards long-term recovery and pain-free feet.