If you’re an active adult dealing with recurring aches, stiffness, or “mystery” joint pain, you’re not broken—and you’re definitely not alone. The real win isn’t giving up activity; it’s learning how to move, recover, and support your body so you can stay active for the long haul.
Why Active Adults Experience Pain
Being active is one of the best things you can do for your long-term health, but it also exposes your muscles, tendons, and joints to repeated stress. When that stress exceeds your body’s capacity to recover, pain is your early-warning system—not a punishment, just a very persistent notification.
Overuse: Too Much, Too Soon, Too Often
Overuse injuries happen when a tissue (like a tendon or joint) is loaded repeatedly without enough time to adapt and recover. Common examples include runner’s knee, Achilles tendinopathy, tennis elbow, and shoulder impingement from repetitive overhead work or sport.
Real-life overuse scenarios:
- You add two extra days of running per week without changing anything else, and your knee starts complaining.
- You discover pickleball, play four days in a row, and suddenly your elbow hates your life choices.
- You decide “this is my year” at the gym, jump from one workout a week to five, and your shoulders and back flare up.
Evidence-based management of overuse emphasizes:
- Relative rest (modifying, not stopping, activity).
- Progressive loading (gradually strengthening the irritated tissue).
- Addressing contributing factors like technique and strength imbalances.
Muscle Imbalances and Weak Links
Most people have muscles that are overworking and others that are underworking, especially around key joints like hips, knees, shoulders, and the core. When stabilizing muscles are weak or slow to activate, bigger muscles and passive structures (tendons, ligaments, joint surfaces) pick up the slack and can become painful over time.
Common patterns:
- Strong quads but weak glutes → knee and front-hip pain with running or stairs.
- Strong pecs and lats but weak mid-back and rotator cuff → shoulder and neck tension.
- Weak deep core and hips → lower back doing more than its fair share.
Aging Joints (Without the Doom Story)
As we age, cartilage naturally thins and joints can develop osteoarthritic changes. That doesn’t automatically mean you’re doomed to pain, but it does mean your joints appreciate smart loading, muscle support, and good mechanics.
Research shows that:
- Strengthening and staying active improves function and can reduce joint pain.
- Simple external supports (like soft knee braces) can moderately reduce pain and improve physical function in knee osteoarthritis.
Tight Muscles and Poor Mobility
When muscles are chronically tight or stiff, they limit joint motion and force other areas to compensate, often leading to pain in the “innocent” area. For example, stiff hips or ankles can push extra stress into your lower back or knees when you walk, squat, or run.
Tightness often comes from:
- Repetitive positions (like sitting all day).
- Repetitive patterns (like always hitting the same workout or sport).
- Lack of regular mobility work and recovery.
Posture and Movement Habits
Posture isn’t about looking like a statue; it’s about how you distribute load across your body over time. Slumped sitting, “tech neck,” hanging into one hip, or always standing with knees locked all alter how joints and muscles share the workload.
Key points:
- No single posture is “perfect”—problems show up when you stay in one position for too long.
- Small changes in how you sit, stand, lift, and walk can significantly change which tissues get overloaded.
Sedentary Work + Intense Exercise: The Modern Combo
Many active adults spend most of the day sitting, then ask their body to perform like an athlete for an hour. That big mismatch—long static sitting plus sudden high loads—is a common recipe for pain.
Typical pattern:
- 8 hours at a desk → hip flexors tighten, glutes and deep core go on vacation.
- Evening run, heavy lifting, or sport → tight, underprepared tissues suddenly asked to do explosive work.
You’re not “too old”; your tissues are just being surprised.
The Most Common Sources of Pain in Active Adults
Recognizing your pain pattern helps you choose the right solutions—not just throw random stretches at the problem.
Lower Back Pain
Lower back pain is one of the most common complaints in active adults, especially those who sit a lot and then train hard. It often shows up as a dull ache, stiffness when you first stand up, or discomfort with prolonged standing, lifting, or bending.
Common contributors:
- Weak or poorly coordinated deep core and hip muscles.
- Stiff hips or thoracic spine, forcing the lower back to move more.
- Poor lifting mechanics, repetitive bending, or unsupported sitting.
Hip Pain
Hip pain may show up in the front of the hip, side of the hip, or deep in the glutes. It often appears with running, walking uphill, squats, or prolonged sitting.
Possible drivers:
- Weak glute med and hip rotators, leading to poor control of thigh position.
- Tight hip flexors from sitting, increasing stress on the front of the hip.
- Overuse of hip flexors and adductors (inside-thigh muscles) with sports or classes that emphasize repetitive forward movement.
Knee Pain
Knees frequently complain in runners, hikers, lifters, and weekend warriors. Pain often appears around or behind the kneecap, on the inside of the joint, or under the kneecap with stairs, squats, or long sitting
Common patterns:
- Patellofemoral pain (pain around/behind the kneecap) from poor tracking and muscle imbalance.
- Tendinopathy (jumper’s knee) from repeated jumping or heavy quad loading.
- Osteoarthritic pain, often with stiffness and discomfort in the morning or after inactivity.
Research indicates that for knee osteoarthritis, soft braces can provide moderate pain reduction and small to moderate improvements in function.
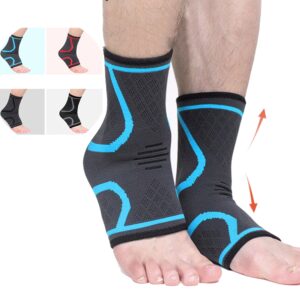
Foot and Arch Pain
Your feet are your foundation; when they’re not happy, everything up the chain can suffer. Common issues include plantar fasciitis (heel or arch pain), achy arches after standing/walking, or forefoot pain.
Contributors:
- Low or high arches without adequate support.
- Sudden changes in activity or surfaces (e.g., treadmill to pavement).
- Tight calves and limited ankle mobility.
- Inadequate footwear or lack of cushioning/support.
Supportive insoles and orthotics can help redistribute pressure, improve alignment, and reduce strain on feet and lower limbs when selected and used appropriately.
Shoulder and Neck Pain
Shoulder and neck pain often arise from a combo of posture, muscle imbalance, and repetitive overhead or forward-reaching activity. Symptoms may include achy upper traps, sharp shoulder pain with lifting, or tension headaches.
Common drivers:
- Rounded shoulders and forward head posture from computer/phone use.
- Weak mid-back and rotator cuff muscles.
- Repetitive overhead lifting or sports (swimming, tennis, pickleball, overhead press) without adequate stability.
The Best Pain Relief Solutions That Actually Work
This is where it gets practical. The best results usually come from combining three pillars:
- Smart movement and strengthening.
- Thoughtful recovery and muscle care.
- Targeted support from braces, posture aids, and insoles.
Think of it as giving your body better software (movement patterns) and better hardware (supports) while also investing in maintenance (recovery).
1. Movement and Mobility: Move Better, Hurt Less
Stretching That Actually Helps
Stretching can reduce short-term stiffness and improve your range of motion, especially when combined with strengthening and active movement. Instead of random “whatever feels tight” stretching, focus on areas that commonly limit movement:
Good targets for active adults:
- Hip flexors (from prolonged sitting).
- Hamstrings and calves (from walking, running, or lifting).
- Chest and lats (from computer and gym work).
- Thoracic spine (mid-back) rotation and extension.
Guidelines:
- Hold gentle stretches 20–30 seconds, 2–4 times per muscle group.
- Keep intensity at “mild to moderate stretch,” not pain.
- Pair stretching with movement (like dynamic warmups) before exercise.
Mobility Work: Teaching Joints to Move Well
Mobility work combines controlled movement and strength at end range to help joints move more freely and efficiently. It’s especially useful for hips, ankles, shoulders, and the thoracic spine.
Examples:
- Controlled circles for hips and shoulders.
- Deep, supported squats for hip and ankle mobility.
- Thoracic spine rotations on the floor or using a foam roller.
Mobility is like giving your joints more “room to negotiate,” reducing strain on surrounding structures during activity.
Strengthening Supporting Muscles
Pain often improves when you strengthen the muscles that guide and stabilize the painful area, not just the area that hurts. Graded strengthening is one of the most evidence-supported approaches for overuse and degenerative pain.
Key strengthening priorities:
- Hips and glutes for knee, hip, and back issues.
- Deep core for back and hip problems.
- Mid-back and rotator cuff for shoulder and neck pain.
- Calves and intrinsic foot muscles for foot/ankle pain.
Principles:
- Start with low to moderate resistance and pain-free or minimal discomfort ranges.
- Progress slowly (e.g., every 1–2 weeks) by adding reps, load, or complexity.
- Aim for 2–3 sessions per week per muscle group.
Research highlights that progressive loading programs (especially for tendons) can remodel tissue and improve pain and function better than prolonged rest.
2. Recovery Techniques: Helping Muscles Let Go
Your body adapts and heals between workouts, not during them. Recovery tools are not “nice-to-have extras”—they’re your long-term pain insurance.
Muscle Release Tools and Targeted Pressure
Self-massage tools (massage balls, lacrosse balls, massage sticks) can apply targeted pressure to tight or tender spots. This may decrease local muscle tension, improve blood flow, and improve mobility.

Best uses:
- Glutes and piriformis (for back/hip issues).
- Calves and plantar fascia (for heel and arch pain).
- Upper back and pecs (for shoulder and neck tension).
Guidelines:
- Apply firm but tolerable pressure for 30–60 seconds on each tender spot.
- Breathe slowly and avoid tensing against the pressure.
- Stay on muscle tissue; avoid directly loading bony areas or joints.
Foam Rolling
Foam rolling is a form of self-myofascial release that can reduce muscle soreness, ease tightness, and improve short-term flexibility. It’s a great add-on before workouts to prep tissues and after workouts to help recovery.
Benefits documented in practice and supported by emerging evidence:
- Eases muscle tension and improves comfort during movement
- Improves range of motion in key muscles like hamstrings and quads
- May reduce perceived soreness and stiffness after intense activity
Safe foam rolling tips:
- Focus on muscles (quads, hamstrings, glutes, calves, upper back), not joints or bones
- Roll slowly (about 1–2 cm per second) for 30–60 seconds per area
- Avoid rolling the lower back or neck; instead, use gentler targeted tools or guided exercises
Massage and Hands-On Care
Manual therapy (massage, joint mobilization, soft tissue work) by a skilled therapist can reduce pain in the short term and improve motion. It’s most powerful when paired with active rehab (strength and movement retraining) rather than used alone.
Think of hands-on work as:
- Unlocking motion and easing tension.
- Creating a “window” where exercise feels easier and more comfortable.
- Not a cure by itself, but a valuable tool alongside movement changes.
3. Supportive Gear That Helps You Move Better
Supportive tools like braces, posture supports, insoles, and muscle release devices are not cheats; they’re load-management tools. Used wisely, they can help you move with less pain while you rebuild strength and mobility.
Knee Braces and Supports
Knee braces can help in conditions like knee osteoarthritis, patellofemoral pain, and mild instability. Research indicates that soft knee braces can have moderate effects on pain and small to moderate improvements in self-reported physical function for knee osteoarthritis.

How they help:
- Redistribute load across the knee joint (especially unloader braces in osteoarthritis)
- Enhance proprioception (your awareness of joint position), which may improve control
- Provide warmth and compression, which many people find soothing
Best uses:
- Walking, hiking, or daily activities that usually provoke pain.
- Early phases of rehab when pain limits confidence and movement.
- Situations where uneven surfaces or longer activity would otherwise be aggravating.
They should support your rehab, not replace strengthening and mobility work.
Back Supports and Belts
Back supports can help by reminding you to maintain more neutral alignment, providing gentle compression, and giving you confidence to move. They can be useful for:
- Heavier or repetitive lifting tasks at work or home.
- Temporary relief during a painful flare-up.
- Long periods of sitting or standing when your back fatigues quickly.
Key point:
- Back supports should be used as a short- to medium-term aid while you build better core endurance, hip strength, and movement patterns—not as a lifelong crutch.
Posture Supports
Posture supports (braces, straps, or smart posture reminders) help gently cue you out of prolonged slouching or forward-head positions. They can reduce strain on the neck, upper back, and shoulders when used alongside active strategies.
How they help:
- Provide gentle tactile feedback when you start to collapse into poor posture.
- Reduce time spent in high-stress positions for the neck and shoulders.
- Complement mid-back and shoulder strengthening work.
They are most effective when combined with:
- Regular movement breaks from sitting.
- Exercises that strengthen mid-back, rotator cuff, and deep neck stabilizers.
Supportive Insoles and Orthotics
Orthotic insoles can redistribute pressure under the foot, support arch structures, and improve comfort in walking and running. They may help with plantar fasciitis, arch pain, and some knee or hip complaints linked to foot mechanics.
How insoles help:
- Provide cushioning to reduce impact stress.
- Support the arch to reduce strain on plantar fascia and Achilles tendon.
- Help align the foot and ankle, potentially reducing stress up the kinetic chain.
Tips:
- Pair insoles with appropriate footwear for your activity.
- Break them in gradually over several days to allow your feet to adapt.
- Combine them with foot and calf strengthening for long-term resilience.
Muscle Release Tools (Rollers, Balls, Sticks)
These tools make it easier to do self-massage and trigger-point release at home or on the go. They’re especially handy for:
- Runners and walkers (calves, quads, IT band area).
- Lifters and desk workers (upper back, pecs, glutes).
- Anyone with “knots” that don’t respond to stretching alone.
Used correctly, they help reduce muscle tension, improve mobility, and support faster recovery between workouts.
Simple Habits That Protect Your Joints (Prevention = The Best Pain Relief)
Once pain calms down, prevention becomes your best strategy. Think of this as building a buffer so daily life and workouts no longer push you over the edge.
Improve Posture (By Moving More, Not Posing)
The goal is posture variety, not posture perfection. Joints and tissues tolerate many positions well—as long as you change them often.
Helpful habits:
- Change sitting positions every 20–30 minutes.
- Keep screens at eye level when possible to reduce neck strain.
- Alternate between sitting and standing if you use a standing desk.
- Use posture supports as a gentle reminder, not a rigid cage.
Upgrade Movement Mechanics
Technique matters. Small changes in how you squat, run, lift, or reach can dramatically change which tissues take the load. Working with a coach, physical therapist, or knowledgeable trainer can help you refine your form.
Key areas to prioritize:
- Hinging from the hips instead of rounding the lower back when bending or lifting.
- Keeping knees tracking over toes (not collapsing inward) in squats, stairs, and lunges.
- Using the hips and core for power instead of relying on the low back.
Build Joint Stability and Strength
Stable joints are surrounded by strong, well-coordinated muscles. You don’t need complicated routines; you need consistency with the right basics.
Core ideas:
- Include 2–3 days per week of strength training for major muscle groups.
- Prioritize single-leg work (step-ups, split squats, single-leg deadlifts) for hip, knee, and ankle control.
- Include balance and control exercises (e.g., standing on one leg, controlled step-downs).
Research emphasizes that addressing muscular imbalances and improving joint stability reduces recurrence of overuse injuries and persistent pain.physio-pedia+1
Maintain Muscle Balance and Flexibility
You can’t out-strength-train completely neglected flexibility and vice versa. Balance both.
Simple routine ideas:
- For every pushing exercise, include a pulling exercise (e.g., pushups + rows).
- Pair heavy or high-intensity training days with focused recovery work (foam rolling, stretching).
- Regularly check in with problem areas: hips, ankles, thoracic spine, and shoulders.
When Pain Needs Medical Attention
Most everyday aches from training, gardening, or work can be managed with activity modification, self-care, and smart supports. But some symptoms are red flags.
You should seek medical attention if you notice:
- Persistent pain lasting more than a few weeks that doesn’t improve with rest and basic self-care.
- Nerve symptoms such as numbness, tingling, burning, or weakness in the limbs.
- Significant swelling, warmth, or visible deformity around a joint.
- A joint that feels unstable, “gives way,” or locks/catches repeatedly.
- Sudden, severe pain after trauma (fall, awkward step, heavy lift).
- Systemic signs like fever, unexplained weight loss, or night pain that doesn’t change with position.
A medical or rehab professional (physician, physical therapist) can:
- Rule out serious conditions.
- Provide a clear diagnosis.
- Guide you in a graded, evidence-based rehab plan tailored to your activity goals.
Quick FAQ: Pain Relief for Active Adults
What is the best pain relief for active adults?
The most effective approach usually combines:
- Activity modification (reducing or tweaking aggravating movements, not stopping everything).
- Targeted strengthening and mobility work for the affected area and surrounding joints.
- Recovery tools (foam rolling, self-massage, stretching).
- Supportive gear (braces, insoles, posture supports) to offload stressed tissues.pubmed.ncbi.nlm.nih+2
Medication can be part of a short-term plan under medical guidance, but long-term relief comes from changing how your body handles load.
How can I relieve muscle and joint pain naturally?
Natural strategies with evidence or strong clinical support include:
- Graded strengthening and movement retraining to restore tissue capacity.physio-pedia+1
- Mobility work and stretching to address stiffness.
- Foam rolling and self-massage to reduce tension and improve comfort.reform-pt+1
- Using braces, supports, and insoles to reduce strain and improve mechanics during activity.pubmed.ncbi.nlm.nih+1
- Optimizing sleep, hydration, and stress management, which all influence pain perception.
Do braces and supports actually help with pain?
Yes, when matched to the right problem and used appropriately:
- Soft knee braces show moderate improvement in pain and small to moderate improvement in function for knee osteoarthritis.
- Certain braces (like unloader knee braces) can significantly improve pain and joint load distribution in selected patients.
- Back and posture supports can reduce strain and improve comfort, especially during tasks that normally aggravate symptoms, when combined with active rehab.
They’re tools to help you move with less pain while you build strength and better mechanics—not a replacement for movement work.
How can I stay active without worsening pain?
Use these principles:
- Respect pain but don’t fear it: keep pain during and after activity at a manageable level (e.g., 0–3/10 that settles within 24 hours).
- Modify, don’t stop: adjust volume, speed, range of motion, or impact level instead of quitting entirely.
- Warm up with mobility and light activation work before you push intensity.
- Use supports (braces, insoles, posture aids) during higher-load activities if certain joints tend to flare.
- Progress training gradually, especially after time off or when adding new activities.
If you had to pick one area to improve first—strength, mobility, or supportive gear—which feels like it would make the biggest immediate difference for you right now?