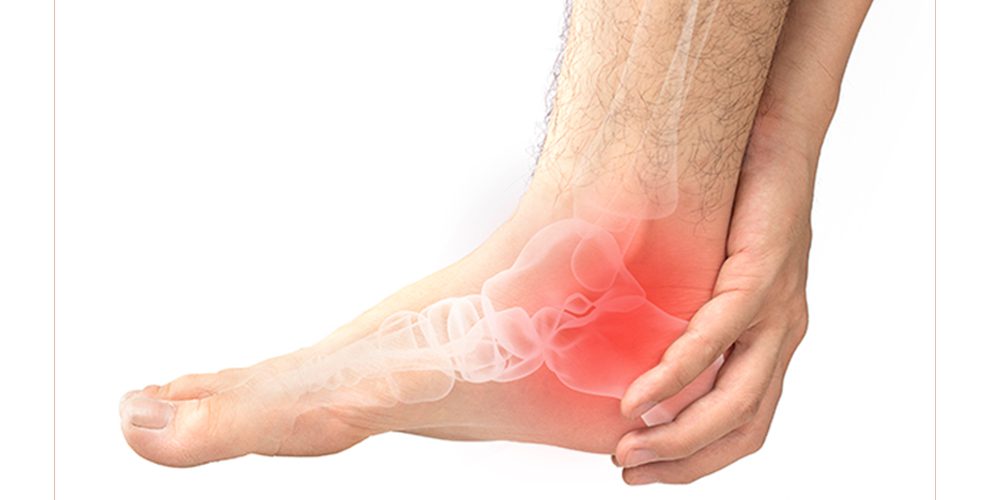
Osteoarthritis is a disease that causes the cartilage in joints to break down, causing pain and eventually limited movement. This condition can be found in many different parts of the body including the foot and ankle. Osteoarthritis in the foot or ankle may cause pain during walking or running, an inability to stand on toes or raise your heel off of the ground.
Symptoms of arthritic feet and ankles
Osteoarthritis is the most common form of Arthritis and millions of people all around the globe are affected. This condition is more and more difficult to treat the more advanced it gets. Common symptoms of OA include:
- Swelling around your joint(s) because of inflammation
- Stiffness, tenderness and discomfort when you apply pressure
- Redness and warmth around your joint(s) during activity
- Increased pain at night
- Decreased range of motion (especially if it only affects one foot)
- Bone spurs (heel spurs)
- Grating, crackling or popping sounds from the joints
- Morning stiffness that lasts longer than 30 minutes after waking up
Osteoarthritis is a leading cause of disability and you should take those symptoms seriously. If you notice any combination of those symptoms above that doesn’t go away, please make sure to contact your doctor or healthcare provider.
Causes of osteoarthritis in foot
Osteoarthritis is caused by the deterioration of cartilage that cushions the ends of your bones’ joints. Cartilage is a tough, slippery tissue that allows for very little friction in moving joints.
Finally, when the cartilage deteriorates entirely, bone will grind against bone.
Osteoarthritis is often referred to as a disease of wear and tear. However, osteoarthritis affects the whole joint beyond the loss of cartilage. It causes alterations in the bone and connective tissues that hold the joint together and connect muscle to bone. It also induces irritation of the joint lining inflammation.
Factors that increase your risk for getting Osteoarthritis include:
- Your Age. The cartilage wears down over time. That means that the older you get, the more prone to getting OA you are.
- Your Gender. It isn’t clear why, but women are more likely to develop OA than men.
- Your Weight. That extra pounds that you collected over the winter contribute to osteoarthritis as well. The higher the weight, the more pressure on the joints. And in addition, fat tissue produces certain proteins that can lead to inflammation in and around your joints.
- Poor posture. A lot of people develop OA because of the way they stand. That’s why it’s crucial to always maintain good posture and protect your back as much as you can.
- Injury or trauma to a joint, such as from a fall or weight-lifting accident. If you break a bone, have surgery or an injury involving certain joints, you’re more at risk for developing OA.
- Joint infection. If you’ve had a joint infection in the past, you’re at risk for developing OA.
- Genetics. Some people are born with genes that make them more likely to develop OA.
- Stress on the joints. Sports like running hiking, playing basketball or dancing place a lot of repetitive stress on your joints. When your job requires frequent kneeling or heavy lifting, that raises your risk for developing OA.
- Medical conditions. Diabetes or different types of arthritis, such as rheumatoid arthritis, increase your risk for developing OA.
Diagnosis
At the beginning of each diagnosis stands a physical exam. During this exam, your doctor checks your joints for stiffness, tenderness, swelling and flexibility.
In most cases, it is important to get pictures of the joints. Your doctor will recommend getting X-rays and MRI. An X-ray can rule out other causes and conditions but doesn’t show cartilage. That’s why MRI (Magnetic resonance imaging) is used in addition. MRI can show the bones and soft tissues, including cartilage.
Besides imaging lab tests may be necessary to confirm the diagnosis. Blood tests are great to rule out other forms of arthritis, such as rheumatoid arthritis. Your doctor might want to draw fluid from your joint with a needle. That procedure is called joint fluid analysis and it is a great tool to determine if your pain might have a different cause other than osteoarthritis.
Osteoarthritis Treatment
Treatments for osteoarthritis in your feet and ankles consists of three different types. Unfortunately, the condition cannot be reversed, so the focus is all about pain management to keep you as mobile as possible.
Medication
Pain relief is the primary goal with medications. For some people, Acetaminophen has helped to reduce the pain to a manageable level. The downside is that taking more than the recommended dose of acetaminophen can cause serious liver damage and complications.
Over-the-counter NSAIDs such as Ibuprofen, naproxen or aspirin typically reduce or relieve the pain from osteoarthritis. If these NSAIDs are not enough, you can get stronger ones with a prescription.
The antidepressant duloxetine has shown some great results in treating chronic pain. And it’s being used in some cases to treat pain from osteoarthritis in the foot and ankle as well.
Therapy for arthritic feet
The very first thing that needs to be done is get a good physical therapist. Physical therapy can help you strengthen your muscles to support your joints better and more effectively, increase stability and flexibility and ultimately relieve pain. Gentle exercises you can do on your own are also recommended. These include swimming and walking, activities that are gentle on the joints.
An occupational therapist can show you how to use little gadgets and helpers to everyday tasks. That is good for reducing the stress on your joints. A bench in your shower is one good example. You don’t need to stand as much while showering and that reduces the pressure on your joints significantly. Different techniques to stand up from a chair, get out of bed or brush your teeth are other examples of what occupational therapy can do for you.
Surgery
As always, surgery is only the last resort if all conservative therapy methods failed.
The first of the common surgery options is cortisone injections. The amount of cortisone injections per year is usually limited to three to four because the medication can further damage the joints over time.
Another type of injection therapy is lubrication injections. Artificial cushioning hyaluronic acid gets injected into your joint and provides more pain relief than cortisone.
Realigning the bones through osteotomy means that your doctor cuts across the bone above or below the joint and adds or removes a wedge of bones. That is a working surgery method if one side of your body is more affected than the other to shift the balance more to the other, healthier side.
Joint replacement is the most complicated method that needs the longest recovery time. Your surgeon removes the damaged joint surfaces and replaces them with plastic or metal parts. Artificial joints might wear out over time and need to be replaced, that is the downside to this procedure.
Lifestyle changes and home remedies for osteoarthritis in the foot
Once you got the diagnosis of osteoarthritis, you need to change your way of life to slow down the process.
Low-impact exercises are good for people with osteoarthritis because they put less stress on the joints. Swimming and water aerobics are excellent exercises because the water supports your body weight. Walking is another good exercise to do if you have time for it. Take a short break after every five minutes of walking to rest your feet. If you’re into cycling, this is another good option for you because it is gentle on the joints, too. Just try some activities and find out what’s good for you and what provides the most fun to you.
Losing weight is always a good idea. But with osteoarthritis, this becomes a necessity if you’re overweight. Extra weight puts more stress on your joints and worsens the condition. Every pound you lose takes four pounds of pressure off your knees.
Hot and cold compresses can provide relief from pain and inflammation. Use a heating pad on low or a hot water bottle for heat, or put ice in a plastic baggie and wrap it in a towel for cold.
Moving stretches like yoga or tai chi can help reduce pain and improve balance. If you already know some of these exercises, do them three to five times a day for 10 to 15 minutes each time.
Getting enough sleep is essential for a good rest. Resting your muscles and joints can reduce or prevent inflammation and swelling.
Ankle or foot braces can be excellent nonsurgical treatments for OA. These devices lower the swelling and pressure on your joints. If you’re looking for a brace that provides more stability for your joints, just have a look at our shop. We have various great options for your feet, ankles or knees.
A nutritious diet is especially important. Not only is it good for weight management, but some types of osteoarthritis also respond to flavonoids that are found in fruits and vegetables. Antioxidants in fruits and vegetables help to combat the free radicals that are responsible for inflammation, cell damage and swelling. There are several great foods that you should integrate into your diet. These include:
- Fish oil
- Green tea
- Ginger
- Curcuma
- Grapes
- Pomegranate
- Pineapple
- All types of berries
- Tomatoes
Takeaways
Osteoarthritis is a condition that affects the joints, causing pain and swelling. It can be difficult to live with this chronic condition, but there are many ways you can manage it to make your life easier. In this article, we’ve covered treatment options like injections or surgery as well as lifestyle changes and home remedies for osteoarthritis in the foot and ankle such as weight loss, exercises for low-impact activities, sleep requirements and diet tips.
We hope you find our suggestions helpful! If you have any questions about how these strategies might work best for your situation or want more information on additional treatments not mentioned here please comment on this article below.
As always, I’d love to hear your stories, tips and lifestyle changes that helped you take your life to a better state.