Picture this: You wake up, ready to conquer the day, only to feel a sharp, stabbing pain in your heel as soon as you take that first step. You try to brush it off, thinking it’ll magically disappear, but alas!
It lingers throughout the day, making walking an agonizing ordeal. Welcome to the world of plantar fasciitis!
So, what exactly is plantar fasciitis? Well, my friend, it’s a condition characterized by inflammation of the plantar fascia – a thick band of connective tissue that runs along the bottom of your foot from heel to toe.
This band acts like a shock absorber for your feet and supports their arches. When subjected to excessive stress or strain, tiny tears can develop in this tissue leading to pain and discomfort.
Prevalence and Common Causes
Plantar fasciitis is more common than you might think! It affects millions of people worldwide and can strike both athletes and couch potatoes alike.
It’s one of the most common causes of heel pain among adults. Now, let’s dig into what causes this pesky condition.
One prevalent culprit is overuse or repetitive stress on your poor feet. Think about those intense workouts or long hours spent standing on unforgiving surfaces – they can take a toll on your plantar fascia.
But that’s not all! Structural abnormalities in your feet can also contribute to plantar fasciitis woes.
If you have flat feet (you know who you are!) or high arches (those fancy ones), these biomechanical imbalances place extra strain on the plantar fascia over time. In addition to overuse and structural issues, factors like obesity, age (yes, getting older has its downsides), and certain occupations that involve prolonged standing can heighten your risk of developing plantar fasciitis.
So, my tender-footed friend, now that we’ve laid the groundwork and discussed the basics, it’s time to delve deeper into the intricate anatomy of your foot. Get ready to explore how this complex structure works and understand the role of our dear plantar fascia in foot mechanics.
Understanding the Anatomy of the Foot
Overview of Foot Structure and Function
When it comes to understanding plantar fasciitis, one must first delve into a fascinating world—the intricate anatomy of the foot. The foot is an incredibly complex structure composed of numerous bones, joints, muscles, ligaments, and tendons working harmoniously to enable us to walk, run, and dance.
These interconnected parts form three main arches in the foot: the medial longitudinal arch (along the inner side), lateral longitudinal arch (along the outer side), and transverse arch (across the midfoot). These arches play a crucial role in distributing body weight evenly during movement.
The foot’s structure includes 26 bones—yes, you read that right—26! These bones are grouped into three main sections: tarsals (including the heel bone), metatarsals (the long bones in the middle), and phalanges (toe bones).
Moreover, there are over 30 joints in our feet that allow for flexibility and mobility. It’s truly remarkable how these joints work together so seamlessly.
Role of the Plantar Fascia in Foot Mechanics
Now let’s zoom in on one critical component: the plantar fascia. The plantar fascia is a thick band of tissue that spans from your heel bone all the way to your toes.
Think of it as a supportive bridge that runs along your foot’s sole. Its primary function is to provide structural support and act as a shock absorber during weight-bearing activities.
During walking or running movements, this remarkable tissue undergoes tension as it supports your body weight and helps maintain proper foot alignment. It also plays an essential role in creating stability within your feet by preventing excessive flattening or overpronation.
However, when excessive stress or strain is placed on this resilient tissue—often due to repetitive activities or poor biomechanics—it can become irritated and inflamed. This is when plantar fasciitis rears its painful head, leading to discomfort that can make walking a seemingly insurmountable challenge.
Understanding the intricate anatomy of your feet and the pivotal role played by the plantar fascia helps elucidate the causes, symptoms, and treatment options for this debilitating condition. By gaining this knowledge, you’ll be better equipped to navigate through the labyrinth of plantar fasciitis and find effective solutions to alleviate your pain.
Symptoms and Diagnosis of Severe Plantar Fasciitis
Experiencing Excruciating Pain While Walking
Plantar fasciitis, when it reaches a severe stage, can cause excruciating pain that makes every step feel like a torturous ordeal. Walking becomes a challenging task as the sharp, stabbing pain intensifies with each movement. The pain is usually most pronounced in the mornings or after periods of rest when the plantar fascia tightens up, making those initial steps truly agonizing.
This debilitating discomfort can extend along the entire arch of the foot and even radiate to the heel or toes. It often feels like walking on shards of glass or hot coals, leaving sufferers desperate for relief.
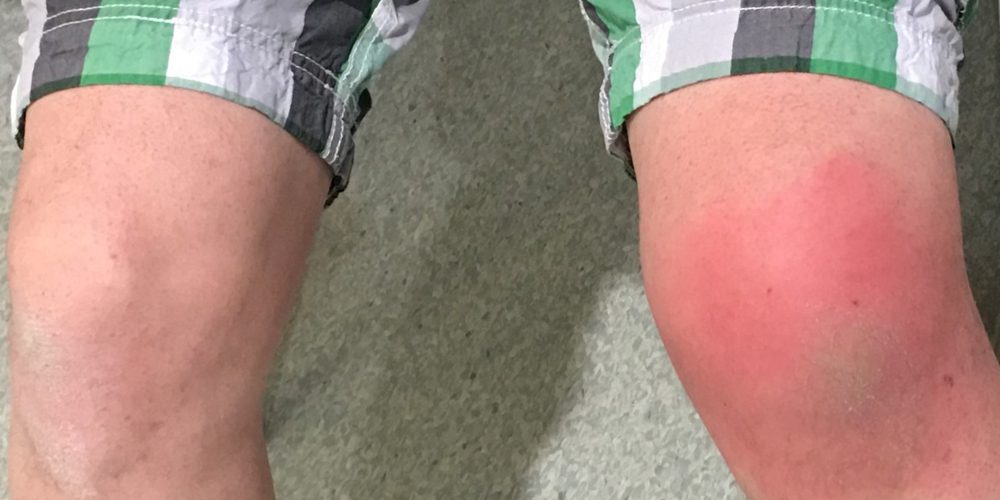
Identifying Other Associated Symptoms (Swelling, Tenderness)
In addition to the intense pain, severe plantar fasciitis may also cause swelling and tenderness in the affected area. Swelling occurs as a result of inflammation in response to micro-tears or degenerative changes within the plantar fascia.
The foot may appear visibly swollen and feel warm to the touch due to increased blood flow in an attempt to promote healing. Tenderness is another telltale sign of advanced plantar fasciitis.
When pressure is applied to specific areas along the arch or heel, it elicits discomfort and sensitivity. Palpating these regions can help identify localized points of tenderness that indicate inflammation and injury within the plantar fascia.
Consulting a Healthcare Professional for Accurate Diagnosis
When experiencing severe symptoms associated with plantar fasciitis, it is crucial to seek professional medical guidance for an accurate diagnosis. While self-assessment can provide an initial indication of potential plantar fasciitis based on symptoms such as excruciating pain while walking, swelling, and tenderness, a healthcare professional will be able to evaluate the condition comprehensively. During a medical consultation, the healthcare provider will typically begin by taking a detailed history of the symptoms, followed by a physical examination.
This examination may involve assessing foot mechanics, checking for any structural abnormalities or imbalances that contribute to plantar fasciitis. The healthcare provider may also apply pressure to various parts of the foot and ankle to identify specific areas of pain and tenderness.
Additionally, diagnostic imaging techniques such as X-rays or ultrasound scans may be recommended to rule out other potential causes of foot pain and to confirm the diagnosis. These tests can provide valuable insights into the extent of damage within the plantar fascia and help guide appropriate treatment strategies.
Remember, accurate diagnosis is essential to develop an effective treatment plan tailored specifically for severe cases of plantar fasciitis. So, it is crucial not to delay seeking professional advice if you are experiencing severe symptoms that hinder your ability to walk comfortably.
Causes and Risk Factors for Severe Plantar Fasciitis
Overuse or Repetitive Stress on the Feet
When it comes to plantar fasciitis, a common culprit is overuse or repetitive stress on the feet. This occurs when you subject your feet to excessive strain and force without giving them sufficient time to rest and recover.
Activities such as running, jogging, or participating in high-impact sports can put immense pressure on the plantar fascia—the thick band of tissue connecting your heel bone to your toes—and lead to inflammation and microtears. So, if you find yourself pushing your limits a little too hard at the gym or constantly engaging in strenuous physical activities, you may be putting yourself at risk of developing severe plantar fasciitis.
Impact of Intense Physical Activities or Sports
Engaging in intense physical activities or sports can be exhilarating, but it also increases the likelihood of experiencing severe plantar fasciitis. Imagine playing basketball with fervor, jumping high to block shots or competing fiercely during an intense match.
These activities involve repetitive movements that place significant strain on your feet and ultimately contribute to the development of this debilitating condition. So, if you are an avid athlete seeking thrills on the court or field, it is crucial to take measures to protect your feet from excessive stress by incorporating proper warm-up routines and wearing appropriate footwear.
Prolonged Standing or Walking on Hard Surfaces
Do you have a job that requires standing for extended periods? Or perhaps you enjoy taking long walks around town? While these may seem like harmless activities at first glance, they can increase your risk of developing severe plantar fasciitis.
Prolonged standing or walking on hard surfaces like concrete puts immense pressure on your feet, leading to fatigue and inflammation of the plantar fascia. So, if your occupation or daily routines involve standing or walking on unforgiving surfaces, it is essential to wear supportive shoes and take regular breaks to give your feet some rest.
Foot Biomechanics and Structural Abnormalities
Our feet are marvels of biomechanics, designed to withstand the pressures of our daily activities. However, certain structural abnormalities can disrupt this delicate balance and contribute to severe plantar fasciitis.
One such example is having flat feet or fallen arches. When you have flat feet, the impact of each step is not adequately absorbed by the arches, resulting in increased strain on the plantar fascia.
Conversely, individuals with high arches tend to distribute weight unevenly across their feet, concentrating pressure on specific areas including the plantar fascia. These biomechanical anomalies can lead to chronic inflammation and pain that make walking a challenge.
Flat Feet or High Arches Contributing to Excessive Strain on Plantar Fascia
Flat feet or high arches can contribute significantly to excessive strain on the plantar fascia, leading to severe plantar fasciitis. Flat feet occur when the arches collapse upon weight-bearing, causing increased tension in the connective tissues that support them.
This puts added stress on the plantar fascia and increases vulnerability to injury and inflammation. On the other hand, individuals with high arches have less natural shock absorption due to reduced surface area in contact with the ground while walking or running.
Consequently, this places excessive load onto specific parts of their foot—including the heel—and heightens their susceptibility to developing severe plantar fasciitis. By understanding these causes and risk factors for severe plantar fasciitis—overuse or repetitive stress on the feet; impact of intense physical activities or sports; prolonged standing or walking on hard surfaces; and foot biomechanics and structural abnormalities such as flat feet or high arches—you can take proactive steps to prevent or manage this debilitating condition.
Remember, caring for your feet is crucial, as they carry you through life’s adventures. So, pay attention to the signs your body gives you and make choices that support the overall health and well-being of your feet.
Treatment Options for Severe Plantar Fasciitis
Conservative measures to alleviate pain and promote healing
When dealing with severe plantar fasciitis that leaves you unable to walk, it is crucial to explore conservative treatment options. These measures aim to provide relief from the excruciating pain while promoting healing of the affected tissues. One effective approach is incorporating stretching exercises into your daily routine.
These exercises specifically target the calf muscles and the plantar fascia, helping to improve flexibility and reduce strain on the foot. Simple stretches like calf raises, towel curls, and toe stretches can make a significant difference in your recovery.
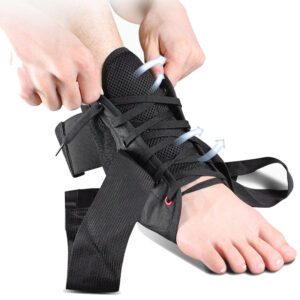
Use of orthotic devices, such as shoe inserts or night splints
Orthotic devices can be a game-changer when it comes to managing severe plantar fasciitis. Shoe inserts, commonly known as orthotics or insoles, play a crucial role in providing additional support and cushioning to your feet. They help distribute pressure evenly and alleviate stress on the plantar fascia.
Night splints are another valuable tool that helps stretch the foot while you sleep by keeping it in a dorsiflexed position. This gentle stretching throughout the night helps relieve morning pain associated with plantar fasciitis.
Application of ice packs or heat therapy for pain relief
When suffering from intense pain caused by severe plantar fasciitis, quick relief becomes a top priority. Applying ice packs or heat therapy can work wonders in soothing discomfort and reducing inflammation around the affected area.
Ice packs help numb the affected region while constricting blood vessels, consequently reducing swelling and alleviating pain temporarily. On the other hand, heat therapy improves circulation by dilating blood vessels and promoting relaxation of muscles and tendons.
Non-steroidal anti-inflammatory drugs (NSAIDs) for reducing inflammation
Non-steroidal anti-inflammatory drugs, commonly known as NSAIDs, are often recommended by healthcare professionals to reduce inflammation and manage pain associated with severe plantar fasciitis. Medications such as ibuprofen or naproxen sodium have anti-inflammatory properties that help alleviate the intensity of discomfort caused by the condition. It is essential to follow the recommended dosage and consult with a medical professional before taking any medication to ensure they are safe for you and do not interfere with any existing conditions or medications.
Combining treatment options for optimal results
While each of these conservative measures provides its unique benefits, combining them can yield even better results in managing severe plantar fasciitis. For example, incorporating stretching exercises into your daily routine along with using orthotic devices can enhance the overall effectiveness of both approaches.
Similarly, alternating between ice packs and heat therapy can provide comprehensive pain relief and reduce inflammation more effectively. Remember that it is crucial to consult a healthcare professional before starting any new treatment regimen to ensure it aligns with your specific needs and medical history.
By implementing these conservative treatment options meticulously and making them a part of your daily routine, you can significantly improve your symptoms and promote healing in cases of severe plantar fasciitis. However, if symptoms persist or worsen despite these efforts, it may be necessary to explore specialized treatments or consult a medical professional for further guidance on managing this debilitating condition.
Specialized Treatments for Persistent Cases
Physical therapy techniques like ultrasound therapy or extracorporeal shockwave therapy (ESWT)
When dealing with persistent plantar fasciitis that hinders your ability to walk, physical therapy can be a game-changer. Among the cutting-edge techniques employed in this field, ultrasound therapy and extracorporeal shockwave therapy (ESWT) have garnered significant attention.
Ultrasound therapy involves using high-frequency sound waves that penetrate deep into the tissues of the foot, promoting blood flow and reducing inflammation. This treatment is administered by trained professionals who move a wand-like device over the affected area, providing gentle warmth and relief.
Over time, ultrasound therapy stimulates natural healing processes within the plantar fascia, helping to alleviate pain and restore mobility. Another effective approach is ESWT, which stimulates healing by generating shockwaves targeted at the affected area.
These shockwaves help break down scar tissue and promote the growth of new blood vessels, accelerating tissue repair. ESWT is typically performed in short sessions over several weeks and has shown promising results in relieving chronic pain caused by severe plantar fasciitis.
Corticosteroid injections to reduce inflammation in severe cases
In some cases where severe inflammation persists despite other treatments, corticosteroid injections may be recommended by healthcare professionals.
These powerful anti-inflammatory medications are directly injected into the affected area of the foot under sterile conditions. Corticosteroids work by suppressing immune responses and reducing swelling within the plantar fascia.
This intervention provides rapid relief from pain and allows individuals to resume walking more comfortably. However, it’s important to note that corticosteroid injections are typically used as a short-term solution due to potential side effects associated with long-term use, such as weakening of the tissues.
Surgical interventions as a last resort
When severe plantar fasciitis persists despite exhausting other treatment options, surgical intervention may be recommended as a last resort. This decision is not made lightly and is usually reserved for cases where all conservative measures have been exhausted and quality of life is severely impacted.
The most common surgical procedure for plantar fasciitis is called plantar fascia release. During this operation, the tight or damaged portion of the plantar fascia is partially or completely released to relieve tension and reduce pain.
Depending on the individual case, surgery may be performed using an open technique or minimally invasive methods involving smaller incisions. While surgery can provide significant relief for individuals suffering from severe plantar fasciitis, it should be approached with caution due to potential risks associated with any surgical procedure.
Recovery time can vary depending on the extent of the surgery and post-operative rehabilitation will likely involve physical therapy to regain strength and flexibility in the foot. Specialized treatments offer hope for those grappling with persistent plantar fasciitis that impedes their ability to walk.
Physical therapy techniques like ultrasound therapy and ESWT leverage technological advancements to stimulate healing within the foot’s tissues. Corticosteroid injections provide rapid relief by targeting stubborn inflammation directly.
Surgical interventions are considered only when all conservative measures have been exhausted, offering a potential solution for severe cases where other treatments have failed. It’s important to consult with healthcare professionals who specialize in foot disorders to determine which approach is best suited for your unique situation.
Lifestyle Modifications to Ease the Pain
Wearing Proper Footwear
When dealing with severe plantar fasciitis, one of the crucial lifestyle modifications is making sure you have the right footwear. Bid farewell to those cute but unsupportive shoes and opt for ones that provide ample arch support and cushioning.
Look for shoes with a firm heel counter, a wide toe box, and good shock absorption properties. Consider investing in orthotic inserts or custom-made shoe inserts to provide additional support and alleviate pressure on the plantar fascia.
Managing Weight and Exercise
Maintaining a healthy weight can significantly reduce strain on your feet. Excess weight puts more pressure on the plantar fascia, exacerbating the pain.
Engaging in low-impact exercises like swimming or cycling can help you stay active without further aggravating your condition. Consult with a physical therapist who can guide you through appropriate exercises to strengthen your foot muscles and improve overall foot stability.
Avoiding Prolonged Standing or High-Impact Activities
Taking frequent breaks from activities that require prolonged standing or walking on hard surfaces is essential for allowing your feet to rest and heal properly. Avoid high-impact activities like running or jumping until your condition improves significantly. If standing is unavoidable, use supportive footwear and consider using gel pads or cushioned mats to reduce impact.
Icing and Stretching
Regular icing of the affected area can help alleviate pain by reducing inflammation. Apply an ice pack wrapped in a thin cloth for 15-20 minutes several times a day.
Additionally, perform gentle stretching exercises targeting both calf muscles and the plantar fascia itself. Stretching helps improve flexibility, reduces tightness, and promotes healing.
Listening to Your Body
Perhaps one of the most important lifestyle modifications is to listen to your body. Pay attention to any warning signs or signals of pain and discomfort.
If an activity or shoe choice exacerbates the pain, modify it accordingly. Remember that healing takes time, so be patient with yourself and adjust your daily routine as needed.
Conclusion
Severe plantar fasciitis can indeed be debilitating, hindering our ability to walk comfortably. However, there is hope for improvement through lifestyle modifications and appropriate treatment.
By wearing supportive footwear, managing weight, avoiding excessive strain on the feet, practicing regular icing and stretching, and being mindful of our bodies’ needs, we can gradually alleviate the pain caused by this condition. Though it may take time and dedication to fully recover from severe plantar fasciitis, adopting these lifestyle modifications can have a significant positive impact on your overall well-being.
Remember to consult with healthcare professionals for accurate diagnosis and personalized treatment plans tailored to your specific needs. Keep in mind that you are not alone in this journey towards healing.
With patience and determination, you will likely regain your ability to walk without excruciating pain. Stay optimistic and committed to making the necessary changes in your lifestyle – brighter days are ahead!